Artificial intelligence (AI) and related technologies keep shaping our society, providing us with more and more solutions that seemed impossible only a few years ago. The medical field is not an exception and nowadays we can realistically discuss the possibilities of AI for drug discovery, the rise of robot radiologists and digitised patients charts for diagnosis. Here we would like to provide some insight through our research as bioinformaticians to show how we are advancing medicine and technologies in contributing to biomedicine digitalisation.

The promise of AI touches every facet of medicine, but unlike some domains in which AI has been applied, in the case of biomedicine we must always be mindful of how crucial a mistake can be.
Translating algorithmic advances to biomedical breakthroughs requires critical consideration of technical aspects and a deep understanding of human biology. For example, we need to understand the true capabilities of new technologies and distinguish them from broad ideas. We have to distinguish between those biomedical problems which can benefit the most from present emerging technologies and others which still have to wait for their time. Finally, taken from an intriguing application case, research is moving towards a systematic change that could actually improve human health.
This relates to one of the most promising applications of AI in medicine, namely the shift from a so-called “one-size fits all” approach towards precision medicine.
Precision medicine vs. ICD
Diseases are commonly diagnosed using International Classification of Diseases (ICD). This classification system is based on symptoms and markers, which commonly describe the disease, but does not cover the individual condition of a patient. The goal of precision medicine is to provide personalised diagnoses and treatments, individually adapted for each patient based on their risk factors, genetics and metabolism. An extensive knowledge about molecular biology and disease mechanisms is necessary to achieve this.
One type of available data, which is crucial in understanding disease mechanisms are molecular interaction networks. Proteins interact with each other to forward signals, genes can be activated or deactivated by so called transcription factors and metabolites are created or broken down to store or provide energy for the cell. These interactions between genes, proteins and metabolites can be represented in networks, similar to railway systems where trains carry goods and people between stations.
Hence, any disease caused by a virus or a mutation in a gene triggers a chain of changes which is propagated through the network. This is one of the reasons why diseases can display many different symptoms which have no clear origin. In simple terms, this could be compared to the cancellation of a train: what we observe is a train being cancelled, but based on this information we cannot say whether: the train itself broke down; the tracks were damaged or blocked; or some failure at a railway station occurred.
Tackling cancer with precision medicine
One application case of AI in medicine is cancer. With almost 20 million newly diagnosed cases and roughly 10 million deaths in 2020, cancer is clearly a major disease burden in today’s world. While early diagnosis and treatment is a key factor for patient survival, it is also extremely difficult for many reasons. On one hand, symptoms can be very unspecific and thereby hard to identify. On the other hand, tumours, even in the same organ, can be very different on a molecular level.
Another important concept in cancer research relates to the so-called driver genes, which trigger tumour development and passenger genes, which are affected once the tumour starts developing.
Coming back to our railway analogy, a driver gene could be the equivalent of a train blocking a hub station. Hence, it affects many other trains and without knowing which caused the initial blockage, it might be not possible to identify the actual cause of delays. Differentiating between cancer drivers and passengers is similarly difficult, but crucial for screening and treatment techniques – just imagine trying to resolve all train delays without knowing where it started.
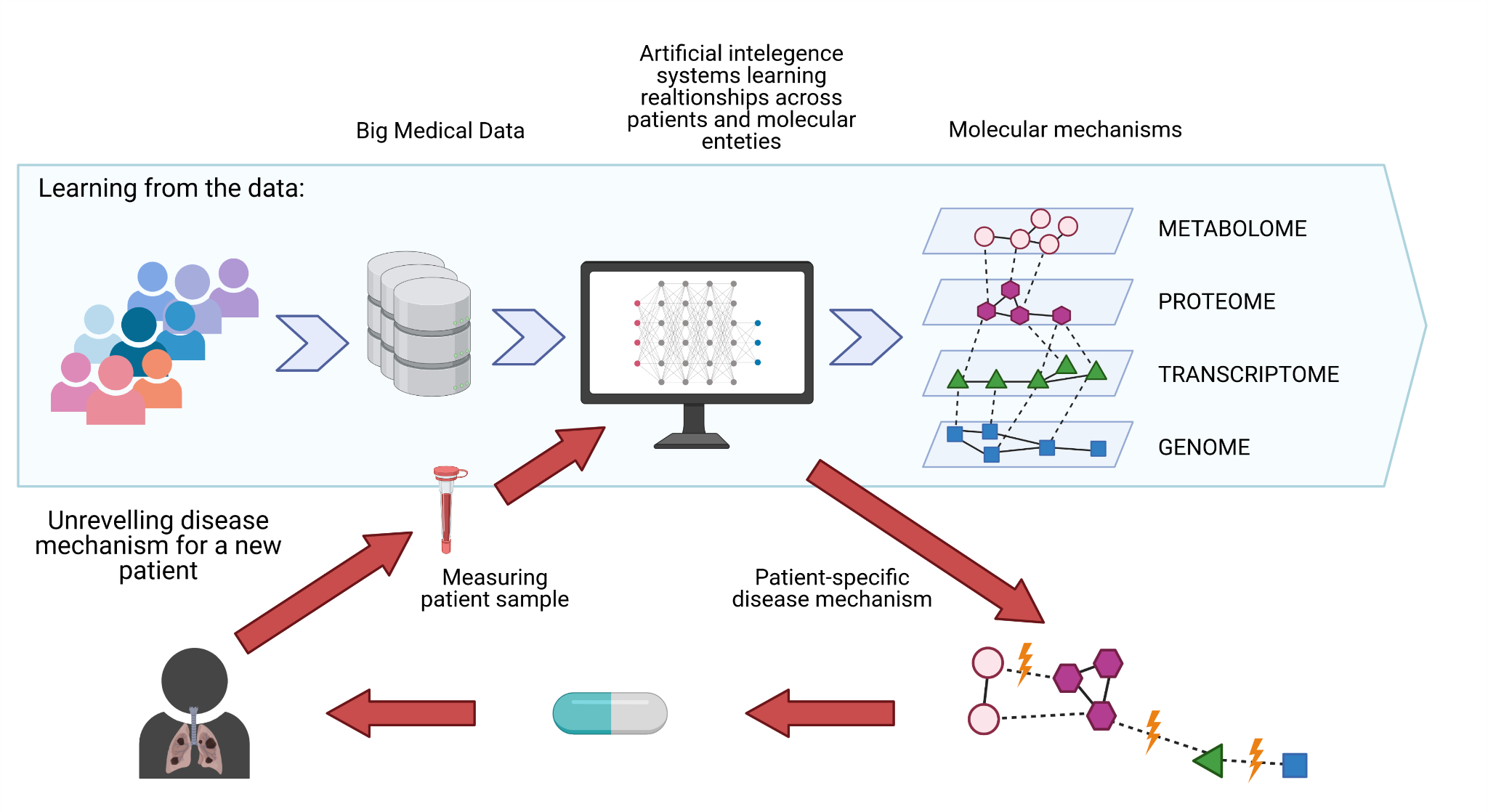
Figure 1: Future of AI in Biomedicine
Created with BioRender.com
Biological research has made huge improvements in recent years, resulting in vast amounts of available data, which can be used by bioinformaticians to develop AI models. In order to provide solutions specific to a tumour’s „individual“ properties, researchers nowadays can use available data about diseases and molecular interaction networks to develop AI models that can comprehend individual differences and disease mechanisms. In this way we can understand how a change in one gene or protein results in systematic changes that lead to a disease. Such methods have been successfully used to identify key-players in liver, bladder, colorectal and blood (leukemia) cancer.
The future of medicine
Modern technologies have profited from digitalisation in the biomedical sector, through which large amounts of patient data are now readily available, facilitating computational cancer research. With the increasing amount of Big Data in medicine, digitalisation is necessary in order to extract insights from (bio)medical data adequately and turn them into clinically relevant discoveries, as manual data analysis is not manageable for thousands and thousands of measurements. Instead of looking at symptoms and applying testing just for disease markers, algorithms could reveal the molecular reason for a disease from a blood probe or biopsy, providing doctors with the information to apply treatments individually for each patient. Future advances in bioinformatics hold great potential for digitalising medicine and improving the health of each individual patient.
The blogs published by the bidt represent the views of the authors; they do not reflect the position of the Institute as a whole.

Nikolai Köhler is PhD candidate in the bidt Junior Research Group LipiTUM at the Technical University of Munich (TUM) holding a Master’s Degree in Molecular Biotechnology from TUM. In his doctorate he is focussing on computational methods for the analysis of metabolite data and metabolic networks in a systems biology context.

Olga Lazareva is bidt Doctoral Fellow in the Chair of Experimental Bioinformatics at the Technical University of Munich (TUM). Holding Master’s Degree in Data Science and Bachelor’s in Mathematics. Funded for DigiTYPE project that aims to develop personalised diagnostics and treatment using AI and biological networks.

Tim Rose is PhD candidate in the bidt Junior research group LipiTUM at the Technical University of Munich. He has a Master from the Humboldt University in Berlin in Biophysics and a Bachelor in Quantitative Biology from the Heinrich-Heine-University in Düsseldorf. He is interested in the computational analysis and simulation of the lipid metabolism.
Passend zum Thema
Research: Same symptom – different cause?
Machine learning is playing an ever-increasing role in biomedical research. Scientists at the Technical University of Munich (TUM) have now developed a new method of using molecular data to extract subtypes of illnesses. In the future, this method can help to support the study of larger patient groups.
Blog: 3D printed human organs – only a Sci-Fi dream?
Imagine a world in which you could simply 3D print a new, customised organ tailored to your very own physiology. At the moment, this is merely a dream for all the people suffering from organ shortages. However, within the field of bioprinting, scientists around the world are working towards the feasibility of 3D printing functional organs using digital fabrication methods. (Englisch)



